FIBROIDS & MYOMECTOMY
What are fibroids?
Fibroids are a common benign (non-malignant) tumour of the muscle and fibrous tissue that make up the bulk of the uterus. They are present in 20% of women of reproductive age and in up to 50% of women over the age of 35 years. They can occur anywhere in the uterus, from the fundus at the top down to the cervix. They also vary in their actual position in the uterine wall.
Fibroids can grow beneath the smooth outer peritoneal covering of the uterus (subserous fibroids), within the depths of the muscle wall (intramural fibroids), or beneath the lining endometrium of the uterine cavity (submucous fibroids). When there are multiple fibroids they are not restricted to one area of the uterus but are usually at all three sites.
How do I find out if I have fibroids?
The fact that you have a fibroid uterus may come as a complete surprise to you when you are told about it at your clinic. The uterus is found to be enlarged and sometimes considerably so. If fibroids grow rapidly they can become massive looking very much like a six-month pregnancy! If there is just a single fibroid, the uterus will feel smooth and enlarged. But often fibroids are multiple which makes the uterus feel very irregular, hard and knobbly. Big fibroids can feel like a hard grapefruit with several hard apples and walnuts all stuck together!
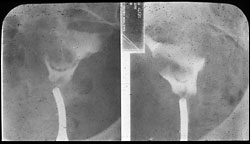
The presence of fibroids is usually first picked up by abdominal and pelvic examination. The diagnosis can be confirmed by ultrasound scan. A hysterosalpingogram (HSG) X-ray can demonstrate a "filling defect" within the uterus (as shown above) and an irregularly shaped cavity instead of the normal smooth outline to the cavity (see Hysterosalpingography information). The technique of hysteroscopy allows the cavity of the uterus to be examined using a fine telescope which is introduced via the cervix. Submucous fibroids are easily recognisable. Both HSG and Hysteroscopy are out-patient examinations.
When there is uncertainty about the cause of a uterine mass, an MRI scan takes images of the uterus. The size and position of any fibroids can be clearly shown. The MRI can also diagnose a form of endometriosis (called adenomyosis) affecting the muscle of the uterus. This is particularly helpful as adenomyosis can produce similar symptoms to fibroids but a myomectomy would not be appropriate treatment. You may develop symptoms which raise the suspicion of fibroids.
What symptoms do fibroids cause?
Subserous fibroids are usually the ones that can reach a very large size. They may not cause any symptoms at all until you can feel a firm lump in the lower abdomen. If they grow out on a stalk (a pedunculated fibroid), they can occasionally become twisted causing severe pain and vomiting. Sometimes fibroids outgrow their blood supply and severe pain commences, rather like a heart attack in the fibroid. This is called degeneration.
Intramural fibroids may cause infertility if they grow large enough and apply sufficient pressure to obstruct the fallopian tubes as they pass through the muscle of the uterus. Their sheer size can press against and distort the shape of the cavity of the uterus.
Submucous fibroids will distort the uterine cavity and actually increase the surface area of the endometrium lining that is shed during each period. As a result periods may become very heavy (menorrhagia) and painful (dysmenorrhoea) with the passage of clots and episodes of flooding. This in turn can lead to anaemia and tiredness. Submucous fibroids can grow to tennis ball size and become pedunculated, eventually passing through the cervix into the vagina. This can be accompanied by severe pain and haemorrhage. From a fertility point of view, submucous fibroids can interfere with the normal implantation of an embryo and be a cause of recurrent miscarriages.
Sometimes fibroids are diagnosed for the first time at the booking ultrasound scan through your antenatal clinic. Fibroids can grow very quickly in pregnancy due to the high levels of oestrogen hormone. Fibroids are associated with preterm labour and preterm rupture of membranes. The babies may be “small for dates”. If fibroids arise in the lower part of the uterus (particularly the rare site of the cervix) it is easy to appreciate how they may prevent the baby's head from entering the pelvis and cause a malpresentation or even obstruct delivery. When fibroids are large there is an increased likelihood of delivery by Caesarean Section.
How do fibroids cause infertility?
Fibroids cause infertility in three chief ways: Compression of one or both fallopian tubes Distortion of the shape of the uterine cavity Interference with normal implantation
Should I have my fibroids removed?
If fibroids are small and not producing any symptoms at all and are not thought to be a factor in your infertility, it is best that they are left alone. They should however be reviewed periodically as they can grow in size until the menopause (“change of life”).
In someone whose family is complete, troublesome large fibroids are best removed with the uterus by means of hysterectomy. This procedure is obviously not in your best interests if you are infertile!
Infertility imposes some obvious restrictions on the type of treatment that is chosen to treat your fibroids. If a particular treatment carries a significant risk of causing further fertility problems, it should be reserved for the woman whose family is complete.
When fibroids are very large there is a significant risk of haemorrhage at any operation to remove them. The fibroids themselves can stimulate the growth of further blood vessels thereby increasing the blood flow through them. It is possible over a period of 6 months to shrink the fibroids dramatically. This involves the use of a drug that suppresses your menstrual cycle by "down regulating" your pituitary gland (see IVF information) and lowers the production of oestrogen. These so called "Gonadotropin-Releasing Hormone (GnRH) Agonists" can be administered as a daily nasal spray or as a monthly or 3-monthly injection. Because oestrogen production is suppressed you may experience menopausal symptoms such as hot flushes, night sweats etc. The effect on the growth of the fibroids may be temporary or permanent. The fibroids will not disappear with this treatment and can start grpwing again when treatment stops. Sometimes your specialist will recommend a course of this hormone treatment before carrying out a myomectomy operation to reduce the risk of haemorrhage occurring during surgery.
Uterine artery embolisation (UAE) is a treatment that is carried out by an interventional radiologist. It is performed under local anaesthetic and sedation. During UAE a tiny catheter is inserted into the femoral artery in the groin and guided under X-ray control to the uterine arteries which are the main blood supply to the uterus. Fine particles of PVA (Poly Vinyl Alcohol) are injected along the catheter. These particles block the blood flow to the fibroids leading to their shrinkage and a significant improvement of symptoms for the majority. UAE needs to be very carefully considered as the effect on fertility is uncertain. There is a small risk of subtly damaging the ovaries leading to premature ovarian failure. Although many women have had successful pregnancies following UAE, there is at present insufficient evidence to ensure its safety for women with infertility.
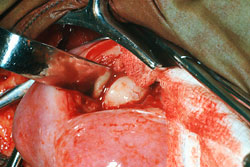
Myomectomy
Myomectomy is the operation to remove fibroids from the uterus without removing the uterus itself.
There are 3 major forms of myomectomy:
- Hysteroscopic myomectomy
- Laparoscopic myomectomy
- Abdominal myomectomy
Fibroids greatly increase the blood supply to the uterus. Because of the risk of haemorrhage during myomectomy, it is essential that cross-matched blood is available in case the need for transfusion arises.
Hysteroscopic myomectomy
Using an operating hysteroscope (resectoscope) quite large submucous fibroids can be removed via the cervix.
Laparoscopic myomectomy
At laparoscopy the fibroids are viewed and additional small incisions are made through which special laparoscopy operating instruments can be inserted.
Pedunculated subserous fibroids can easily be removed laparoscopically. It is also possible to remove multiple subserous fibroids via this route. Intramural fibroids are difficult to access.
Abdominal myomectomy
When fibroids are very large or are intramural, they are best removed via the abdominal route. Even large fibroids can usually be removed through an incision below the bikini line. If fibroids are huge better access may be obtained though a vertical incision.
The aim is to remove every fibroid from the largest to the tiniest, repair the uterus and restore it as near as possible to normal shape and size. Using the minimum number of incisions in the uterus, the fibroids are easily shelled out of their capsules. It is important to open the cavity of the uterus in order to be able to remove any submucous fibroids that could be distorting the uterine cavity. Each cavity left after the removal of a fibroid is closed in layers with dissolving stitches. Sometimes it is necessary to remove some of the over-stretched wall of the capsule that had originally surrounded the fibroid in order to bring about a satisfactory repair. Usually after the myomectomy and repair, the supporting ligaments of the uterus are very lax and need to be tightened. This hitches up the uterus and prevents it from tilting dramatically backwards.
Laparoscopic versus abdominal myomectomy
Both forms of myomectomy are major operations.
The main advantages of the laparoscopic route are that several small incisions are made instead of a single large incision and the post-operative recovery time is quicker. While laparoscopy is ideal for the pedunculated fibroid this is not the case for intramural fibroids.
If there are multiple fibroids, some are likely to be intramural. An open abdominal operation has significant advantages. The surgeon is able to feel small seedling fibroids that would otherwise be missed. (Seedling fibroids will eventually grow into larger fibroids.) Better closure of each fibroid cavity and repair of the uterus can be achieved via the abdominal route.
There are operative techniques that can be employed during abdominal myomectomy that can significantly reduce the risk of haemorrhage. Because of the risks of haemorrhage, the specialist will warn you that sometimes the only way to literally “turn the tap off” is to carry out a hysterectomy. This drastic step is very rarely necessary and would obviously be a disaster from the point of view of your fertility. A hysterectomy would be a last resort life-saving measure.
If you should achieve a pregnancy after an extensive myomectomy operation, there is every likelihood that a Caesarean Section will be recommended as the method of delivery. This is because the incisions that have been made in the uterus may be regarded as potential weak spots which might give way when you are in labour.
There is no guarantee that every fibroid can be removed. Some women require more than one myomectomy operation, particularly those who have fibroids that grow rapidly.
